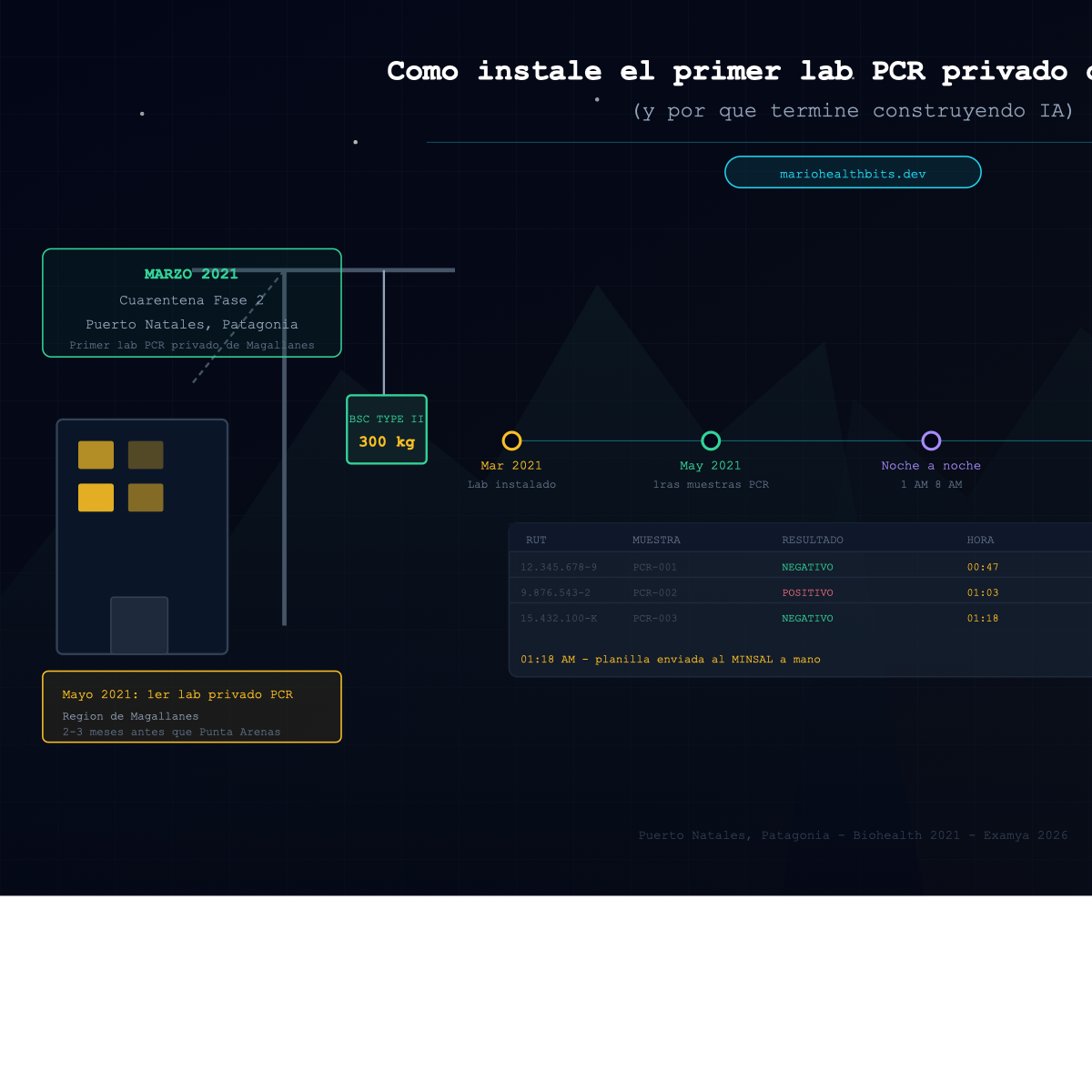
How I Built Patagonia's First Private COVID PCR Lab (And Why I Ended Up Building AI)
In March 2021, I hoisted 300 kg of biosafety cabinet by crane to a second floor during lockdown. By May we were running the first private COVID PCR tests in Chilean Patagonia. The nights that followed became the real origin of Examya.
Mario Inostroza
March 2021. Phase 2 lockdown. Puerto Natales, Chilean Patagonia.
Outside the building, covered in tarps, sat a Type II biosafety cabinet. It had been there for almost a month — 300 kilograms of steel and glass that had traveled thousands of kilometers to reach the lab… and couldn’t get in.
The second floor had only one solution: a crane. In the middle of a pandemic, we hired a crane to lift the equipment up. The same operation we’d need again the day we wanted to take it out.
What nobody tells you about setting up a lab in Patagonia
Building a molecular biology laboratory during lockdown isn’t just science. It’s extreme logistics, creative financing, and a personal bet that could go very wrong.
We pulled the money from three sources: bank loans, Secotec (Chilean government funding), and personal savings. We didn’t have enough capital on our own. We were betting everything we had, at a moment when nobody knew how long the pandemic would last or whether it would be worth it.
The Type II biosafety cabinet and the nucleic acid extractor waited outside for a month, exposed to the Puerto Natales winter, while we figured out how to get them up. Anyone who knows Patagonia knows what that means.
The numbers
By May 2021 we were processing the first COVID PCR samples.
We were the first private laboratory validated to run COVID PCR testing in the entire Magallanes Region. Labs in Punta Arenas, the regional capital, arrived 2-3 months later.
We ended up processing samples from Punta Arenas. Different health services were sending us samples because we were the most efficient in the region. We even traveled to Punta Arenas to run on-site operations, because demand exceeded shipping logistics.
From Puerto Natales. The ones who came later were asking us for samples.
What we actually built
It wasn’t just the lab. It was the team.
We trained people from zero in molecular biology techniques. We learned to lead under real pressure, with results that impacted real people’s treatment, with no margin for error. Crisis teaches things no management course can.
We built protocols. Operational capacity. Team resilience. None of that appears in any clinical lab paper.
The invisible cost: spreadsheets until 1 AM
Here’s the gotcha that never makes it into the success stories.
Every PCR result had to be logged. Full traceability: who took the sample, when it arrived, who processed it, result, time, validation. All by hand. In Excel spreadsheets. Sent to MINSAL systems that didn’t talk to each other.
We finished at 1:00 AM.
We started again at 8:00 AM.
No automation. Everything was human, manual, repetitive, and critical at the same time. One error in a spreadsheet could mean a lost result. And during a pandemic, that had real consequences for real people.
For weeks, the last image of the day was an Excel sheet with rows of ID numbers and results. The first image in the morning, the same sheet with the overnight updates.
Why Chile’s health system is still manual
Chile’s health system works today the same as it did in 2021 in many areas. Paper medical orders. Results sent by WhatsApp as photos. Spreadsheets shared by email. Labs that don’t connect with clinical records.
The problem isn’t technological. The technology exists. It’s about integration, incentives, and the will to automate processes that have “always been done this way.”
That friction has a human cost that never shows up in statistics: the medical technologists finishing at 1 AM. The patients waiting for results that have been ready for hours but haven’t been uploaded yet. The doctors making decisions with incomplete information because the traceability system is an Excel spreadsheet.
Examya isn’t a startup idea
That night in 2021, looking at PCR rows in a spreadsheet at 1 AM, is the real origin of Examya.
It didn’t come from a pitch deck. It didn’t emerge from a hackathon. It’s the physical memory of what it feels like when the system makes you the middleware between the data and the doctor who needs the result.
Examya automates exactly that: processes medical orders from WhatsApp, quotes FONASA pricing automatically, generates traceability without spreadsheets. The Shuri agent does in seconds what we did by hand until the early morning hours in 2021.
The COVID lab wasn’t just an achievement. It was the problem Examya exists to solve.
If you’re building in healthcare or have a manual process that should be automated, let’s talk:
📱 WhatsApp: +56962170366 🐦 X.com: @mariohealthbits 🌐 mariohealthbits.dev
Related reading
In this series
Examya: how I built a medical WhatsApp agent that processes exam orders
Technical details of implementing the Shuri agent in Examya, a system for processing medical orders via WhatsApp with FONASA integration.
In this series
pgvector + Embeddings in Production: The Foundation of Medical Reasoning in Examya
Architecture for semantic search and text similarity in production with pgvector, pg_trgm, and real MINSAL data.
In this series
DeepEval: how I measure the quality of my medical agent with objective metrics
How I built an evaluation layer with DeepEval to measure the quality of Shuri, Examya's medical agent. With real data: from 20% to 70% on E2E, custom metrics for Chile's FONASA system, and why gpt-5-nano doesn't work for structured output.